Interoperability. It’s a term that’s been widely discussed in healthcare. While at its core, the term refers to connectedness between systems or products, the implications are much broader. And therein lies the opportunity. Healthcare needs a more encompassing definition of what interoperability could mean on a grander scale.
For example, we talk about interoperability within a single health system or a single geographic region or between entities. But the backbone of today’s definition of interoperability is still the traditional API. And this is an issue—a roadblock, really. Besides the lack of clarification and standardization within federal legislation and mandates, provider and payer organizations are struggling to achieve compliance via APIs, especially regarding privacy and security. Further, implementation and maintenance are proving to be a significant burden on IT leaders since each connection requires building a separate API to meet each entity’s requirements. It’s a drain on resources and finances—both in short supply right now.
Furthermore, APIs are great at establishing connectivity, but aren’t the answer for delivering comprehensive interoperability. Healthcare data, which doubles every 70 to 80 days, still exists in disparate silos among thousands of databases spread across the country, even within individual enterprises. Building individual connections isn’t the answer.
While APIs provide individual connectivity between entities, they aren’t the hoped-for conduit that finally allows us to maximize the potential of the fast-growing landmasses of data we have available.
What healthcare needs—and APIs can’t provide—is a data exchange infrastructure that acts as a network where participants can connect once and then have access to many. Instead of one-to-one connections, a true data interchange network provides a collaborative platform through which organizations can develop joint processes that help the healthcare community communicate more efficiently.
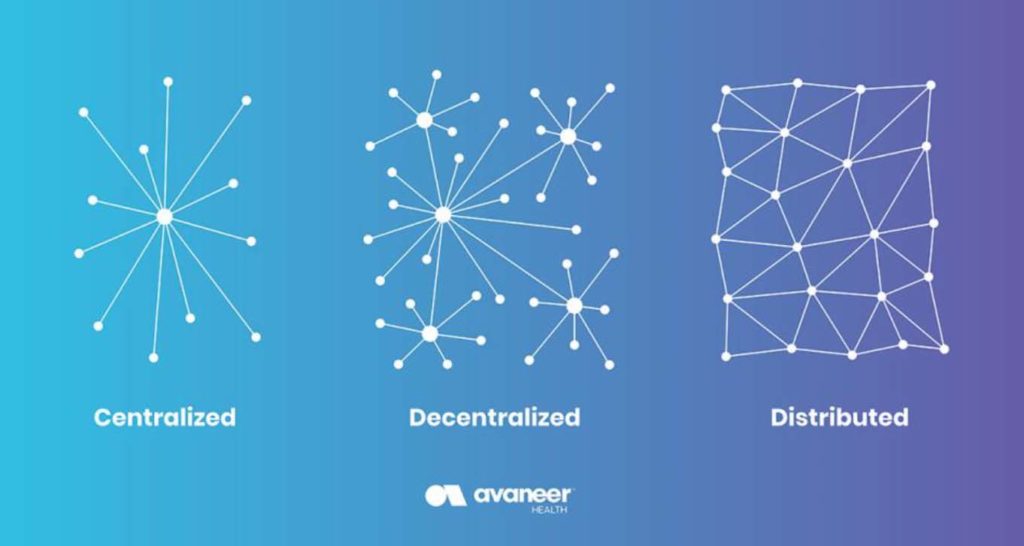
A decentralized, peer-to-peer network makes data interchange possible. Instead of pushing and pulling data through a single gateway between two entities, a network allows access to information among all participants. The potential number of use cases in this type of network is unlimited.
A decentralized, peer-to-peer network enables all participants permissioned access to the same information through a single connection. The network provides secure, tamper-evident storage of transaction data, as well as permission-based access to stored information so that the information can be protected and more reliable and its provenance can be verifiable.
Source: istock
Payers, providers, and third-party vendors who want to participate must agree to allow the data to be discoverable. Members of the network connect via the cloud, where the ID keychain and master index will match the requested data to the available data, then locate the information and deliver it to the requestor. Certifications, cybersecurity, and compliance are all managed by an outside intermediary. Leaders from one of our founding members, Sentara Healthcare, gave their view of how decentralized networks can support transformation within healthcare organizations, read more in the article here.
A decentralized, peer-to-peer network offers unlimited opportunities to advance the quality and efficiency of healthcare delivery in our country. The term “transformative” is not hyperbole here; the potential to transform our industry goes as far as our imaginations can take us.
The broad adoption of APIs and FHIR has been essential in enabling interoperability to move forward into the 21st Century. Up to this point, it’s enabled incremental progress to move us closer to our goals. As technology evolves, we need to leverage a decentralized, peer-to-peer network to eliminate the need for multiple APIs while providing all healthcare stakeholders the ability to work together as a community to build the healthcare ecosystem of the future.