The back-office administration of healthcare is fragmented and full of manual, inefficient processes that impact patient care, provider reimbursement, and costs. These processes are a result of our inability to connect effectively. While payers and providers have invested millions in multiple platforms and legacy systems, many still lack full integration and interoperable functionality.
The annual cost of administrative inefficiencies in the U.S. healthcare system has reached into the billions, with billing, coding, physician administrative activities, and insurance administration being primary drivers.
The challenges of today’s outdated interoperability architecture are significant. From a connectivity standpoint, partner connectivity and workflows require multiple vendors and system integrations. From a data management standpoint, today’s interoperability systems require numerous third parties to support, which has led to a lack of traceability, control, and auditability, as well as security issues. These third parties must aggregate, store, and repurpose data, which means they control the redistribution to payers, providers, and partners. Because of this, payers and providers have little control over when, where, and how they can access it.
Most healthcare organizations have invested in digital and interoperability strategies that, ultimately, have narrow potential and limited scalability. The high costs to maintain connections to multiple third parties require payers and providers to implement and maintain numerous single-use, point-to-point connections.
We now have a web of interconnected systems that don’t easily adapt to evolving trading partner business needs. This has resulted in a wide array of custom, proprietary integration requirements for APIs and third-party platforms—all of which further deteriorate our industry’s quest for interoperability and administrative efficiencies.
Manual transactions, administrative burdens, poor interoperability, and costly and ineffective legacy systems have led to increased total processing spend, provider burnout, poorer outcomes, and limited innovation.
Instead of continuing to add fixes on top of a broken system, healthcare needs to create a new, better system—a system built with a new kind of interoperability.
The term interoperability has different meanings. While we can all agree that sharing data is at the heart of the definition, there are disparities in what that looks like. For example, Fast Healthcare Interoperability Resource (FHIR) has given us a common set of protocols and standards for a payload of transactions on a network. Still, alone, FHIR does not give us full interoperability.
In a truly interoperable healthcare system, data would not need to be requested, aggregated, and validated each time it is needed. Instead, it would be continuously refreshed, always current, and accessible in real time via a secure, decentralized network to those who are permissioned to access it.
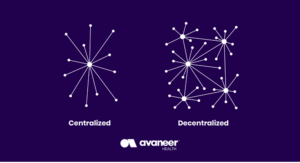
The typical network design consists of a primary server that manages all the information and activities on the network. On a decentralized network, there can be multiple servers acting as primary servers. They each manage information on their own while still connecting with each other. In this way, they “balance the load and distribute the work across the system.” This helps improve network resiliency and data redundancy; if one node goes down, the others are unaffected. Likewise, because data exists in multiple locations throughout a decentralized network, it cannot be changed in one place without changing it across the network.
Benefits a decentralized network can deliver include:
Payers and providers have made progress in improving data accessibility throughout their own enterprises but remain challenged to seamlessly make data accessible between organizations. That lack of data fluidity has led to an industry with a complete lack of transparency that has led to friction, distrust, and data hoarding.
With a decentralized network, payers and providers achieve complete transparency and data fluidity, and they do it without involving third parties. This allows for enriched transactions, providing more actionable patient and procedure-level specificity and clarity. Without a third party, payers and providers require fewer transactions to support operational workflows, while improved data insight supports more effective data management strategies.
This new way of transacting healthcare is not just redesigning current processes. It’s not just about streamlining the way we currently do things. It’s about disrupting how we conduct healthcare and doing things differently. It is about simplifying the business of healthcare.
While we’ve made progress on the road toward interoperability, we have to ask ourselves if our current trajectory can get us where we need to be. Avaneer Health sees a new way forward. We are building a digital ecosystem that accelerates change and enables us to reinvent how healthcare operates. Our decentralized network is now live, and we invite you to join us as we reimagine healthcare together.